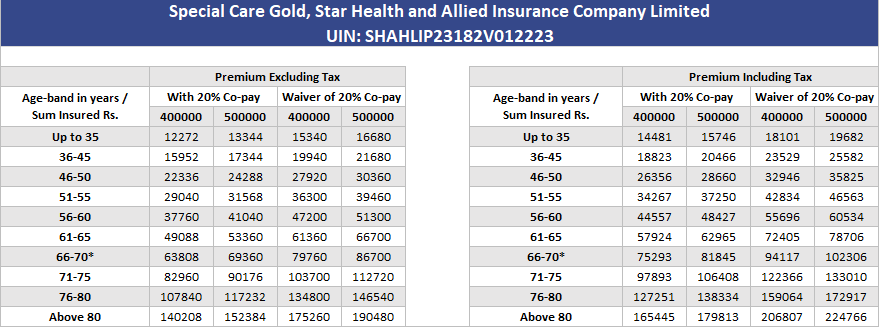
Special Care Gold, Star Health And Allied Insurance Company Limited
Special Care Gold refers to a plan that is particularly designed for individuals with disabilities and those with HIV/AIDS. This initiative of Star Health Insurance for HIV patients and disabled people ensures that healthcare is accessible to all, specifically for people affected by diseases and disabilities. Nowadays, many families also look for reliable health coverage for individuals with disabilities.
Star Special Care Gold provides comprehensive coverage for policyholders with features such as AYUSH treatment, Inpatient hospitalisation, pre- and post-hospitalisation, emergency road ambulance, and so on. This plan is tailored for disabled individuals and HIV-positive patients, offering benefits like low premiums, a wide network of Hospitals, inpatient hospitalisation, Daycare procedures, Cashless treatment, a Policy for the Disabled, Lifetime Policy Renewal, Ambulance Charges, Tax Benefits, and other additional benefits.
Special Care Gold insurance plan is necessary as it provides comprehensive medical coverage and offers features like cashless hospitalisation to people with disabilities and HIV/AIDS. Thus, it provides financial security and peace of mind. As this special policy targets individuals with disabilities (PWD) and those living with HIV/AIDS, it addresses the unique healthcare needs of these groups. In some cases, individuals with disabilities and those living with HIV/AIDS may find it difficult to meet the financial burden of healthcare costs at that time with this health insurance plan. Individuals can search online to find comprehensive health insurance for disabled individuals.
IRDAI UIN: SHAHLIP23182V012223
HIGHLIGHTS
Plan Essentials
Entry Age
Pre-Policy Medical check-up
AYUSH Treatment
Modern Treatment
Instalment Options
DETAILED LIST
Understand what’s included
IMPORTANT HIGHLIGHTS
Unique PlanSpecially designed policy for the persons with a disabilities as per The Rights of Persons with Disabilities Act, 2016 Or / and for individuals with HIV/AIDS as defined under the Human Immunodeficiency Virus and Acquired Immune Deficiency Syndrome (Prevention and Control) Act, 2017. |
Policy TypeThis policy provides benefits only on an individual basis. |
Policy TermThe policy can be taken for a term of 1 year. |
Sum InsuredThe Sum Insured options under this policy are Rs.4,00,000/- and Rs. 5,00,000/-. |
ELIGIBILITY
Disability CoverThe coverage under this policy is available for persons with the following disability/disabilities as defined under the Act and any subsequent additions/modifications to the list in the Act.
Disability for the purpose of this policy means a person with 40% or more of a specified disability as Certified by the Certifying authority as per the Disability Act 2016.
1. Blindness 2. Muscular Dystrophy
3. Low vision 4. Chronic Neurological conditions
5. Leprosy Cured persons 6. Specific Learning Disabilities
7. Hearing Impairment (deaf and hard of hearing) 8. Multiple Sclerosis
9. Locomotor Disability 10. Speech and Language disability
11. Dwarfism 12. Thalassemia
13. Intellectual Disability 14. Haemophilia
15. Mental Illness 16. Sickle Cell Disease
17. Autism spectrum disorder 18. Multiple Disabilities including deaf/ blindness
19. Cerebral Palsy 20. Acid Attack victim
21. Parkinson's disease |
HIV CoverThis policy is available for individuals with HIV/AIDS as defined under the Human Immunodeficiency Virus and Acquired Immune Deficiency Syndrome (Prevention and Control) Act, 2017. Individuals diagnosed as HIV/AIDS by a duly qualified Medical Practitioner with a CD4 count above 350 will only be eligible for cover under this policy. |
HOSPITALISATION CARE (INCLUDING DISABILITY AND HIV/AIDS COVER)
In-Patient HospitalisationHospitalisation expenses incurred for more than 24 hours of hospitalisation are covered. |
Room RentRoom, boarding and nursing expenses all inclusive as provided by the Hospital/Nursing Home are covered up to 1% of the Sum Insured per day. |
ICU ChargesIntensive Care Unit (ICU) charges/Intensive Cardiac Care Unit (ICCU) charges all inclusive as provided by the Hospital/Nursing home are covered up to a maximum of 2% of the Sum Insured per day. |
Pre-HospitalisationIn addition to in-patient hospitalisation, the medical expenses incurred up to 30 days before the date of admission to the hospital are also covered. |
Post-HospitalisationPost-hospitalisation medical expenses including consultation fees, diagnostic charges, medicines and drugs as recommended by the Hospital / Medical Practitioner are covered up to 60 days from the date of discharge from the hospital. |
Emergency Road AmbulanceAmbulance charges are covered up to the maximum of Rs. 2000/- per hospitalisation. |
Day Care ProceduresMedical treatments and / or surgical procedures that require less than 24 hours of hospitalisation due to technological advancements are covered. |
Cataract TreatmentExpenses incurred for Cataract treatment are covered up to Rs. 40,000/- per eye in one policy year. |
Co-paymentEach and every claim under this policy shall be subject to a Co-payment of 20% applicable to the claim amount admissible and payable as per the terms and conditions of the policy. |
Waiver of Co-paymentWaiver of co-payment is available on payment of additional premium as per terms & conditions. |
LUMPSUM COVERAGE FOR HIV/AIDS
Lumpsum Coverage for HIV/AIDSIn case the CD4 count of the insured is/goes below 150, then the Company will pay 100% of the Sum Insured or the balance Sum Insured available under the policy, whichever is lower, as a lumpsum amount to the insured. This payment will trigger after a waiting period of 90 days from the commencement date of the policy.
Note: The claim mentioned above shall be payable once in the lifetime of the insured person and shall not be necessarily linked to an in-patient hospitalisation claim made under the policy. |
WAITING PERIOD
Pre-existing DiseasesI) Applicable for Diseases other than Disability/HIV/AIDS: The expenses related to the treatment of pre-existing diseases and their direct complications are covered after a waiting period of 36 months of continuous coverage after the date of inception of the first policy with the insurer.
II) Applicable for HIV/AIDS: The expenses related to the treatment of HIV/AIDS and its direct complications are covered after 90 days of continuous coverage from the date of inception of the first policy with the insurer.
III) Applicable for Disability: The expenses related to the treatment of pre-existing disability and its direct complications are covered after 24 months of continuous coverage after the date of inception of the first policy with the insurer. |
Specific DiseaseThe expenses related to the treatment of listed conditions, surgeries and treatments are covered after a waiting period of 24 months of continuous coverage after the date of inception of the first policy with the insurer. |
Initial Waiting PeriodThe expenses related to the treatment of any illness within 30 days from the first policy commencement date are excluded except for claims arising due to an accident. |
STAR HEALTH
Why Choose Star Health Insurance?
As a Health Insurance specialist, we extend our services from offering tailor-made products to fast in-house claim settlements. With our growing network of hospitals, we ensure easy access to fulfill your medical needs.
Wellness Program
Diagnostic Centres
E-Pharmacy
GET STARTED
Be Assured of the Best
Get your future secured with us.
Want more information?
Ready to get your policy?
Special Care Gold
What is Special Care Gold, Star Health and Allied Insurance Company Limited?
Special Care Gold, Star Health and Allied Insurance Company Limited is a specialised health insurance plan offered by Star Health Insurance, catering to fulfilling the unique medical needs of individuals with disabilities and those with HIV/AIDS. It is designed to meet the needs of individuals who require extra care due to health conditions. Designed with affordability and accessibility, it provides comprehensive coverage, including hospitalisation expenses, pre- and post-hospitalisation care, and more.
This plan is tailored for individuals who require specialised healthcare coverage. It is crafted to accommodate the health criteria of individuals with HIV-positive/ Aids and disabilities.
The policy aims to help individuals with special needs or disabilities, providing access to comprehensive healthcare services without financial burden.
In India, both HIV prevalence and disability rates are critical public health concerns, each requiring customised responses. Health Insurance can play a crucial role in a context where both HIV and disabilities often lead to social stigma and economic hardship.
Special Care Gold is a unique offering particularly designed for individuals with disabilities and those living with HIV/AIDS. This initiative aligns with Star Health’s core mission to ensure that first-class health care is accessible to everyone, specifically for those affected by diseases and disabilities.
The policy is crafted in accordance with the Rights of Persons with Disabilities Act, 2016, as amended from time to time. It extends coverage to individuals with HIV/AIDS as highlighted under the Human Immunodeficiency Virus and Acquired Immune Deficiency Syndrome (Prevention and Control) Act, 2017, as amended from time to time.
Eligibility for a Disability cover:
Health insurance for disabled persons in India provides financial aid for medical needs. It covers a person with 40% or more of a specified disability, and the disabilities covered under this plan are:
- Blindness
- Muscular Dystrophy
- Low vision
- Chronic Neurological Conditions
- Leprosy Cured Persons
- Specific Learning Disabilities
- Hearing Impairment (deaf and hard of hearing)
- Multiple Sclerosis
- Loco-motor Disability
- Speech and Language disability
- Dwarfism
- Thalassemia
- Intellectual Disability
- Haemophilia
- Mental Illness
- Sickle Cell disease
- Autism spectrum disorder
- Multiple Disabilities, including deaf/ blindness
- Cerebral Palsy
- Acid Attack victim
- Parkinson's disease
Some families also look for health insurance for Parkinson's patients in India because this condition demands long-term medical care and routine medical support.
Eligibility for HIV cover:
Individuals diagnosed as HIV/AIDS by a duly qualified Medical Practitioner with a CD4 count above 350 will only be eligible for cover under this policy.
- Sum Insured options available under this plan are Rs. 4 Lakhs and Rs. 5 Lakhs.
- The Room Rent and ICU/ICCU expenses can be covered up to 1% and 2% respectively, of the Sum Insured chosen.
- This plan covers all day care procedures, with Cataract expenses covered up to Rs. 40,000 per eye in a policy year.
- Special Care Gold’s additional coverages include emergency road ambulance expenses, modern treatments, AYUSH and pre- and post-hospitalisation expenses.
- A Co-payment of 20% is applicable for all admissible claims.
- Customers can waive the Co-payment by paying an additional premium.
- This plan also provides a lump-sum coverage for HIV / AIDS if the CD4 count of the Insured is/goes below 150 with a waiting period of 90 days.
Special Care Gold, Star Health and Allied Insurance Company Limited Benefits
The benefits of buying health insurance for people with disabilities are:
- Coverage for Special HIV Patients: Special Care Gold offers coverage for medical expenses related to the treatment and care of individuals with special needs or disabilities, including consultation fees, therapies, medications, medical equipment, etc. From therapies to all the hospitalisation costs, the plan has you covered.
- Low Premiums: The insurance for HIV patients' price and the insurance for disabled persons' premiums under this plan are tailored to be affordable and accessible. Unable to comprehend “consult the insurance gold plan premium chart”
- Wide Network of Hospitals: Beneficiaries can receive cashless treatment at Star Health's network hospitals.
- In-patient Hospitalisation: The Special Care Gold covers in-patient hospitalisation expenses, such as room rent, operating theatre charges, nursing charges, doctor's fees, ICU charges, and more.
- Daycare Procedures: Under this plan, individuals with disabilities receive medically necessary daycare treatments.
- Cashless Treatment: Individuals can avail themselves of cashless treatment at Star Network hospitals across India.
- Policy for the Disabled:The plan also serves as insurance for disabled individuals, providing essential healthcare coverage.
- Lifetime Policy Renewal: There is an option for Lifetime Policy Renewal, which means that Policyholders can renew the policy for a lifetime.
- Ambulance Charges: Reimbursement of ambulance bills for transporting the insured person to the hospital or from the hospital to the home during a medical emergency.
- Tax Benefits: Premiums paid toward the insurance gold plan premium are eligible for tax benefits as per Section 80D of the Income Tax Act, 1961.
- Additional Benefits: The Special Care Gold offers a Wide Range of benefits, including pre- and post-hospitalisation expenses, daycare procedures, consultation fees, doctor fees, and many more.
Waiting Periods and Exclusions
While the Special Care Gold offers several advantages, it is significant to know its waiting period and exclusions.
Key Points of Waiting Periods:
- Coverage for HIV/AIDS starts after 90 days from policy inception.
- Pre-existing conditions like disabilities are covered after 24 months.
- Other pre-existing diseases have a waiting period of 36 months.
Here are some of the Exclusions:
- Obesity treatments, cosmetic surgeries, and gender transition procedures are excluded from it.
- Injuries from war, hazardous activities, or illegal acts are not covered.
- Experimental treatments are excluded.
Thus, Special Care Gold, Star Health, and Allied Insurance Company Limited have been brought out in line with Star Health’s founding value of making quality health care accessible to specially-abled individuals by empowering them to manage their health with confidence and ease.
People Also Search For
HELP CENTRE
Confused? We’ve got the answers
We’re Star Health. We offer the coverage that’s designed to help keep you healthy. It's the care that comes to you, and stays with you.
Health Insurance Coverage for pre-existing medical conditions is subject to underwriting review and may involve additional requirements, loadings, or exclusions. Please disclose your medical history in the proposal form for a personalised assessment.
The information provided on this page is for general informational purposes only. Availability and terms of health insurance plans may vary based on geographic location and other factors. Consult a licensed insurance agent or professional for specific advice. T&C Apply. For further detailed information or inquiries, feel free to reach out via email at marketing.d2c@starhealth.in